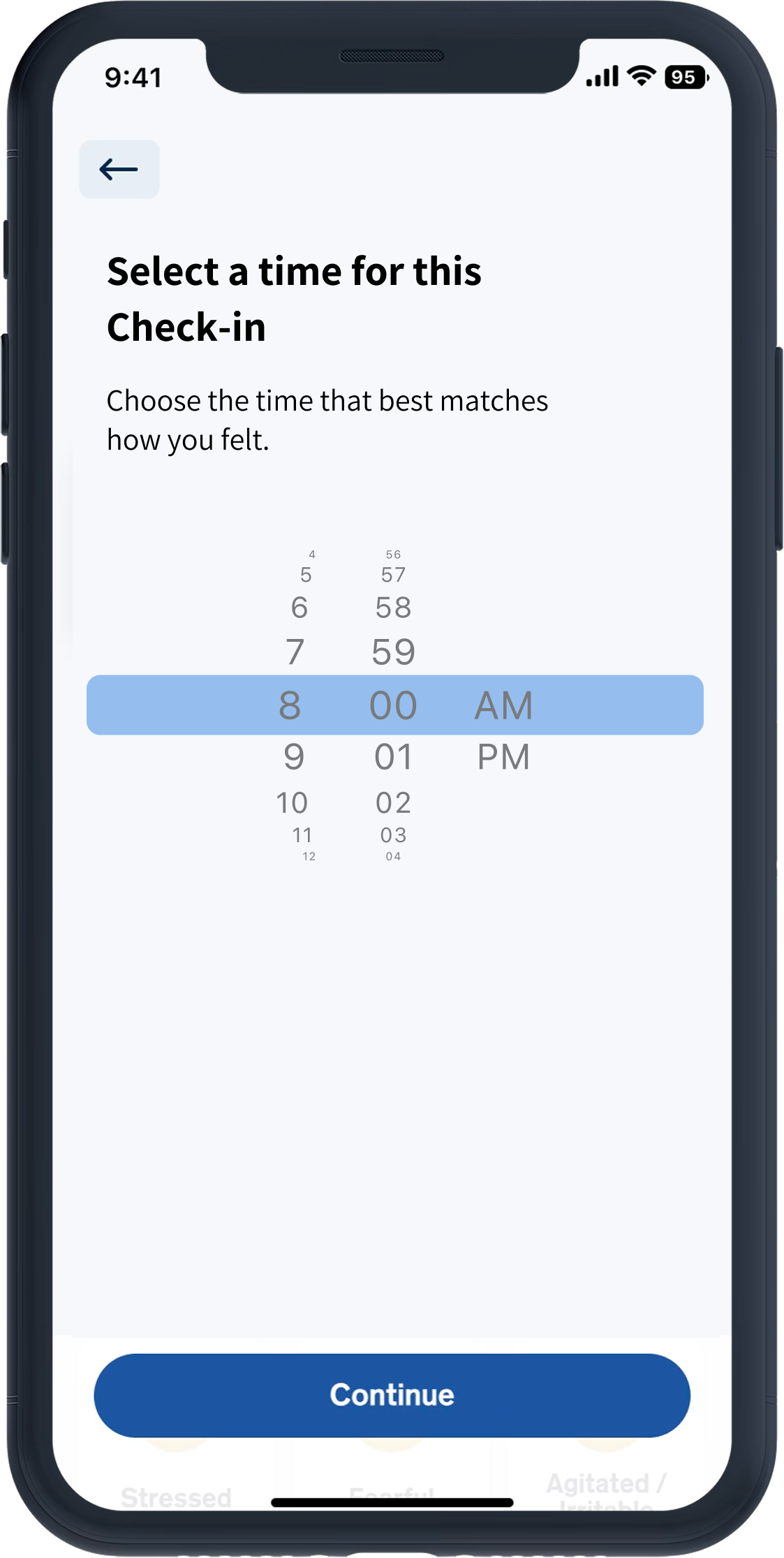
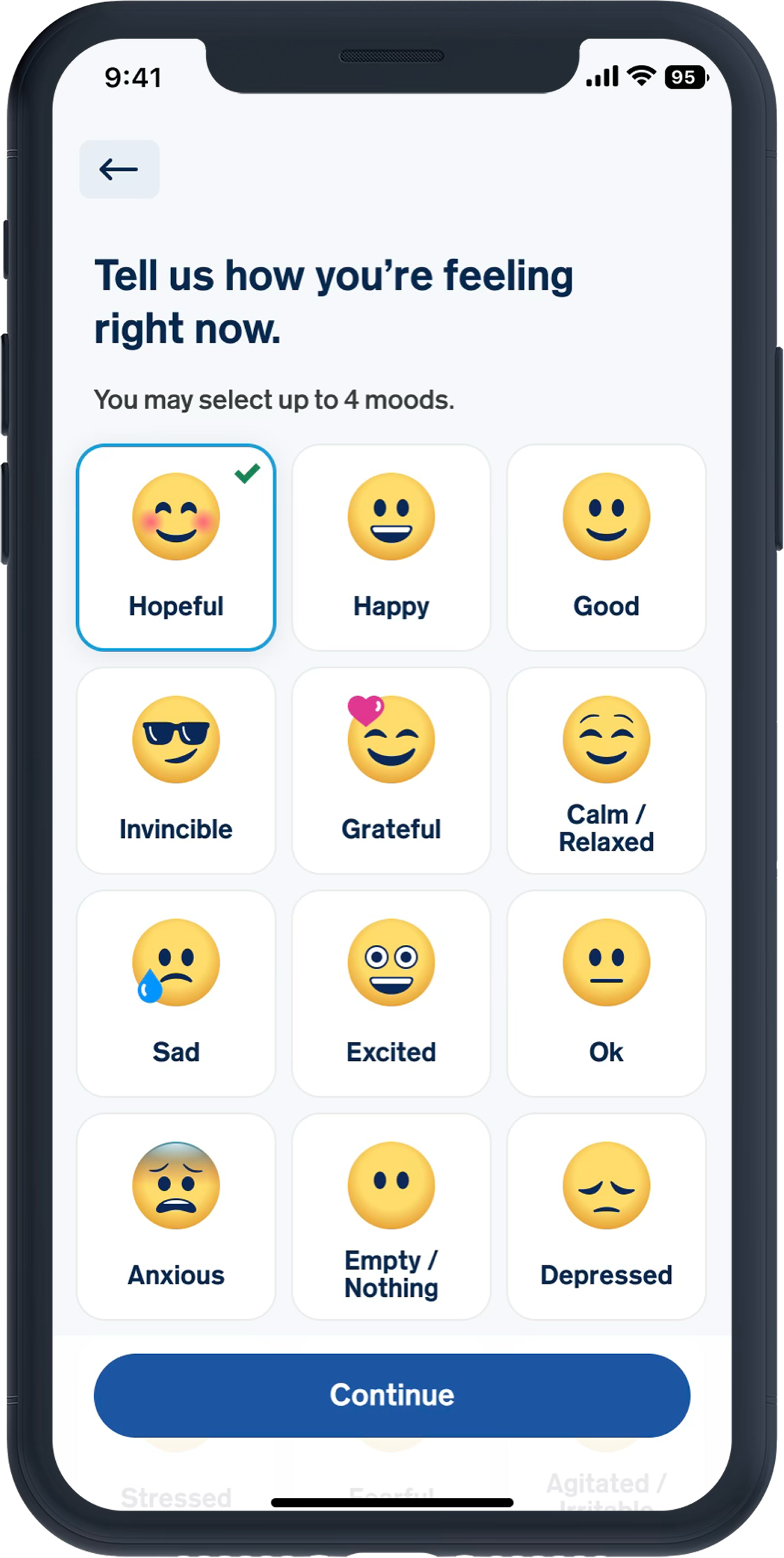
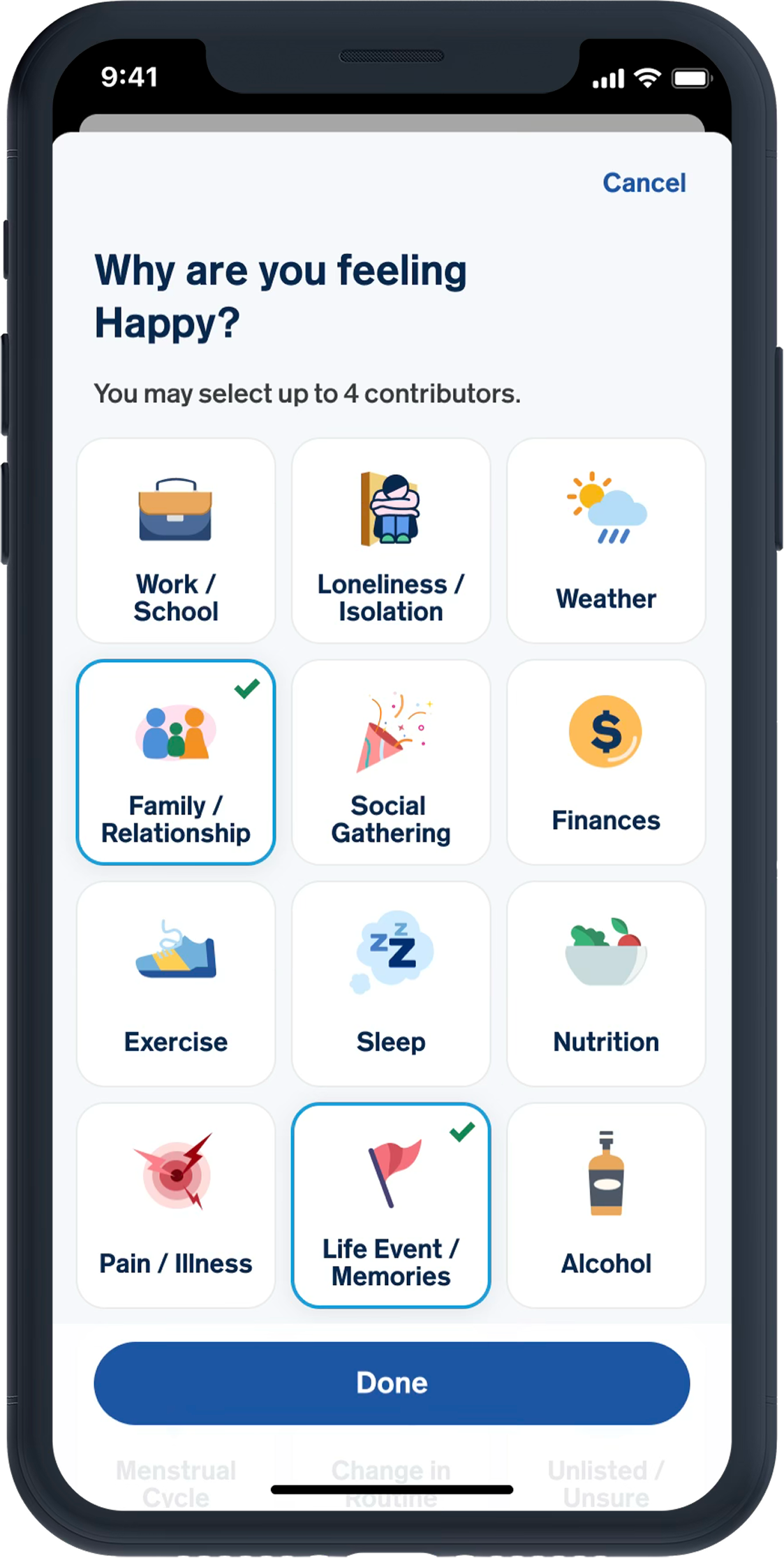
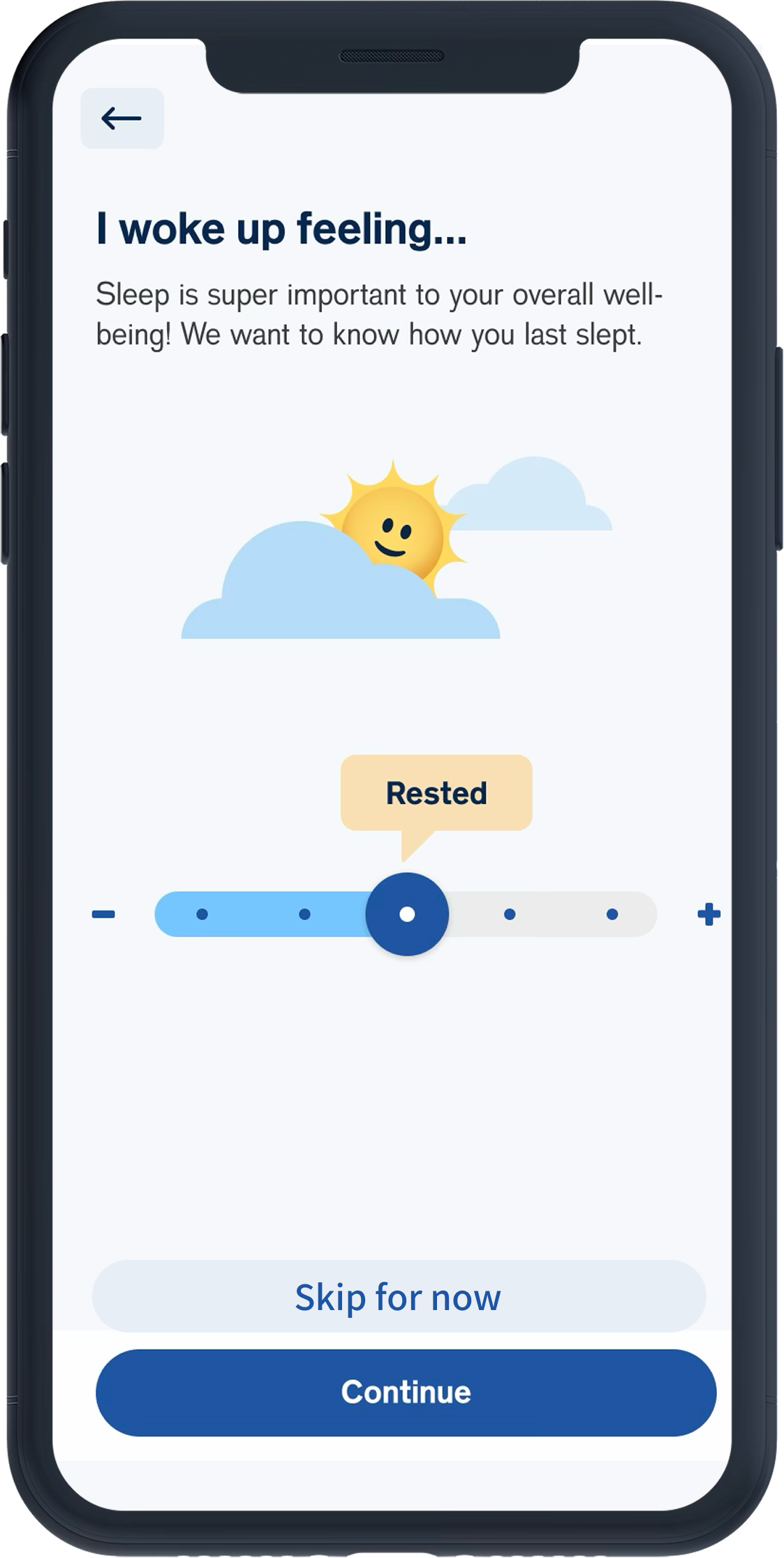
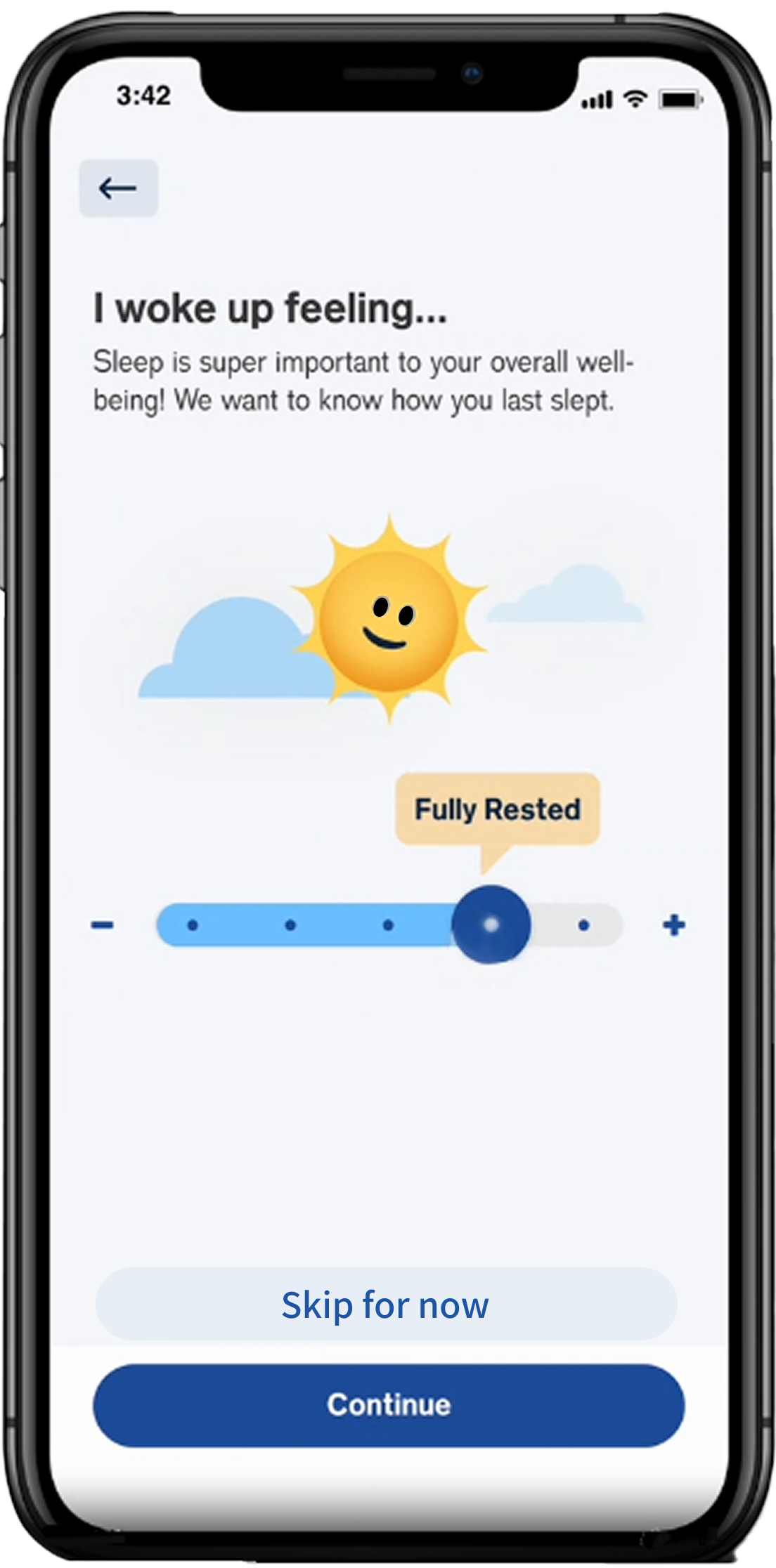
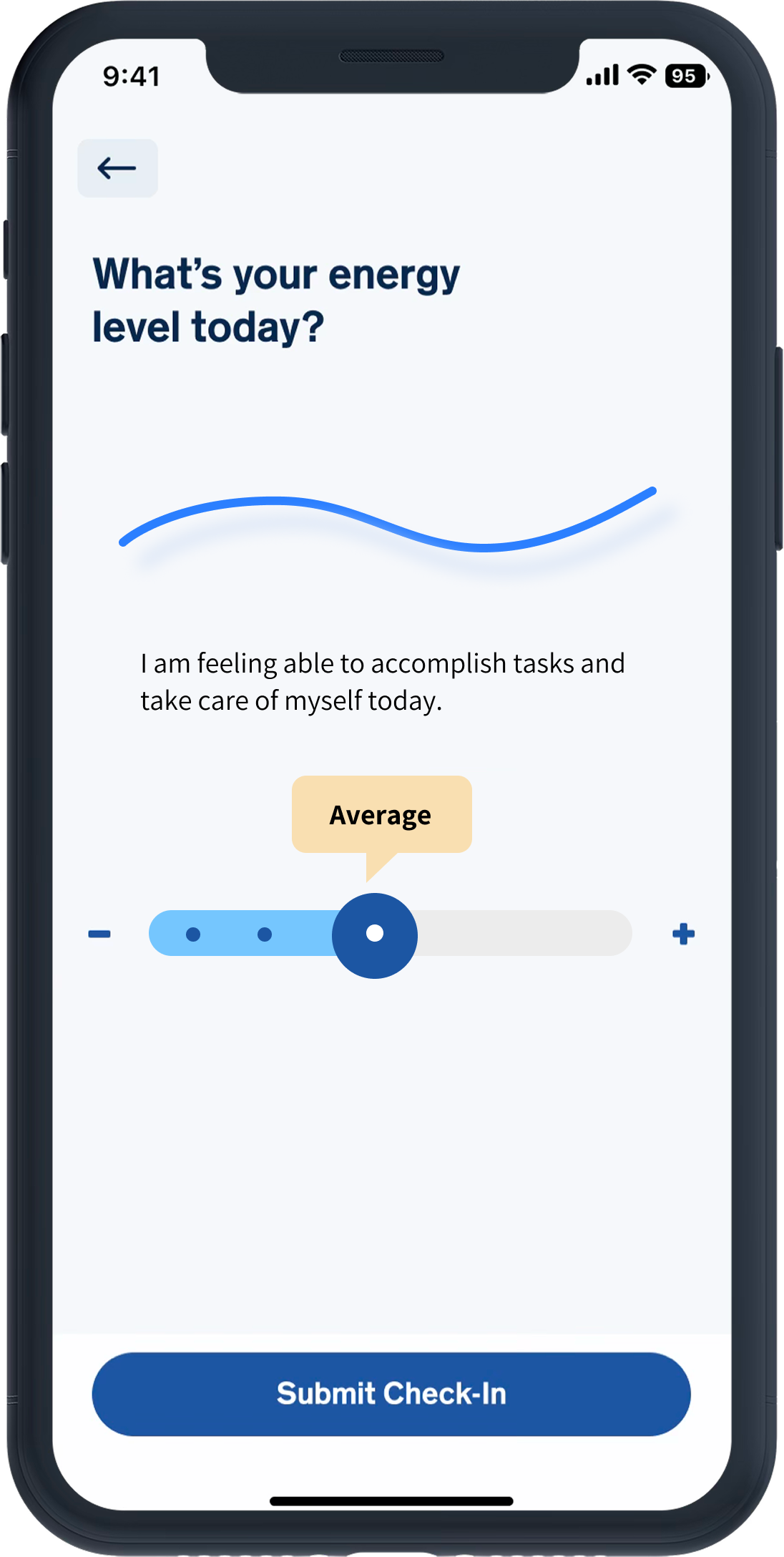
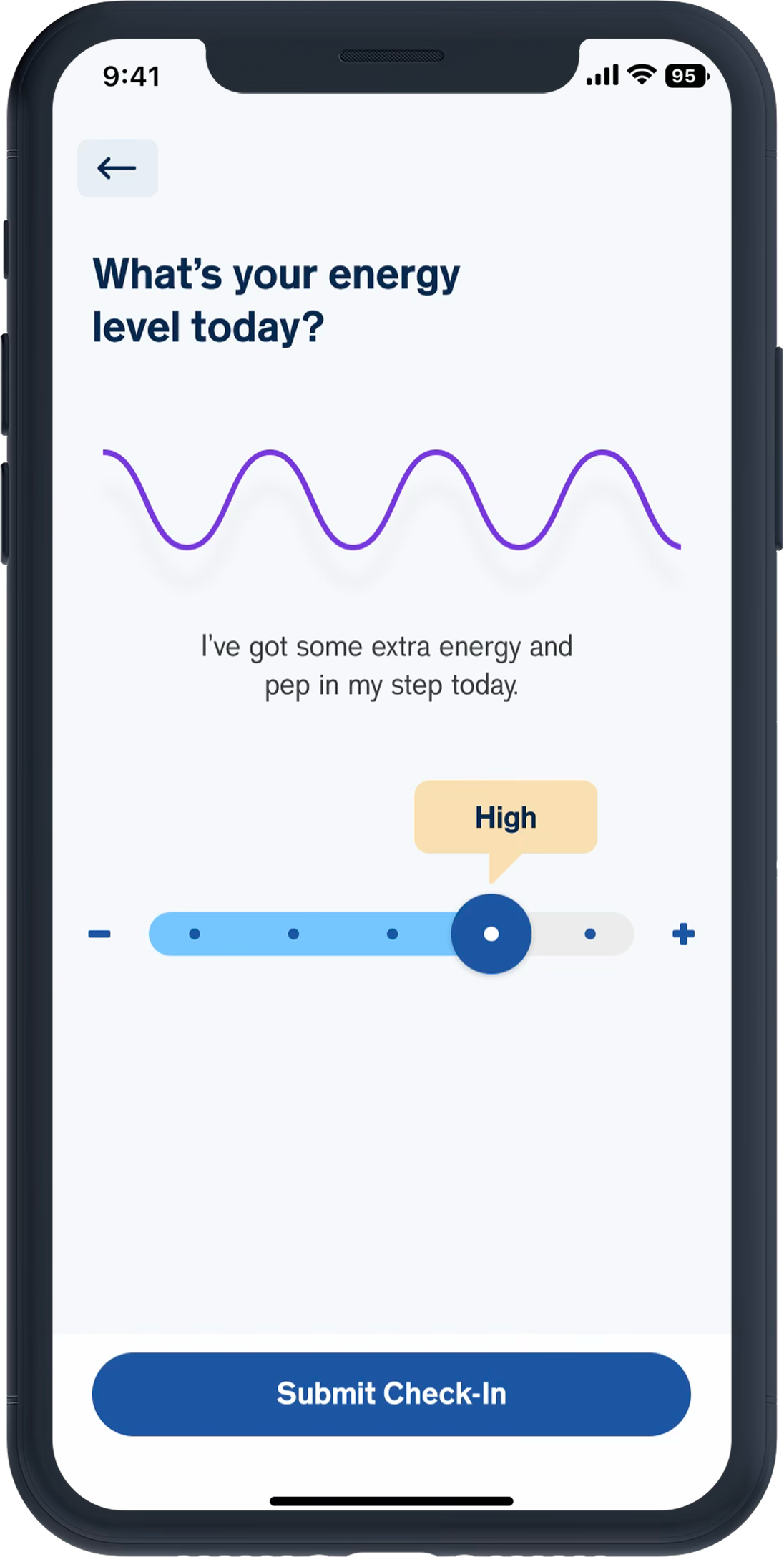
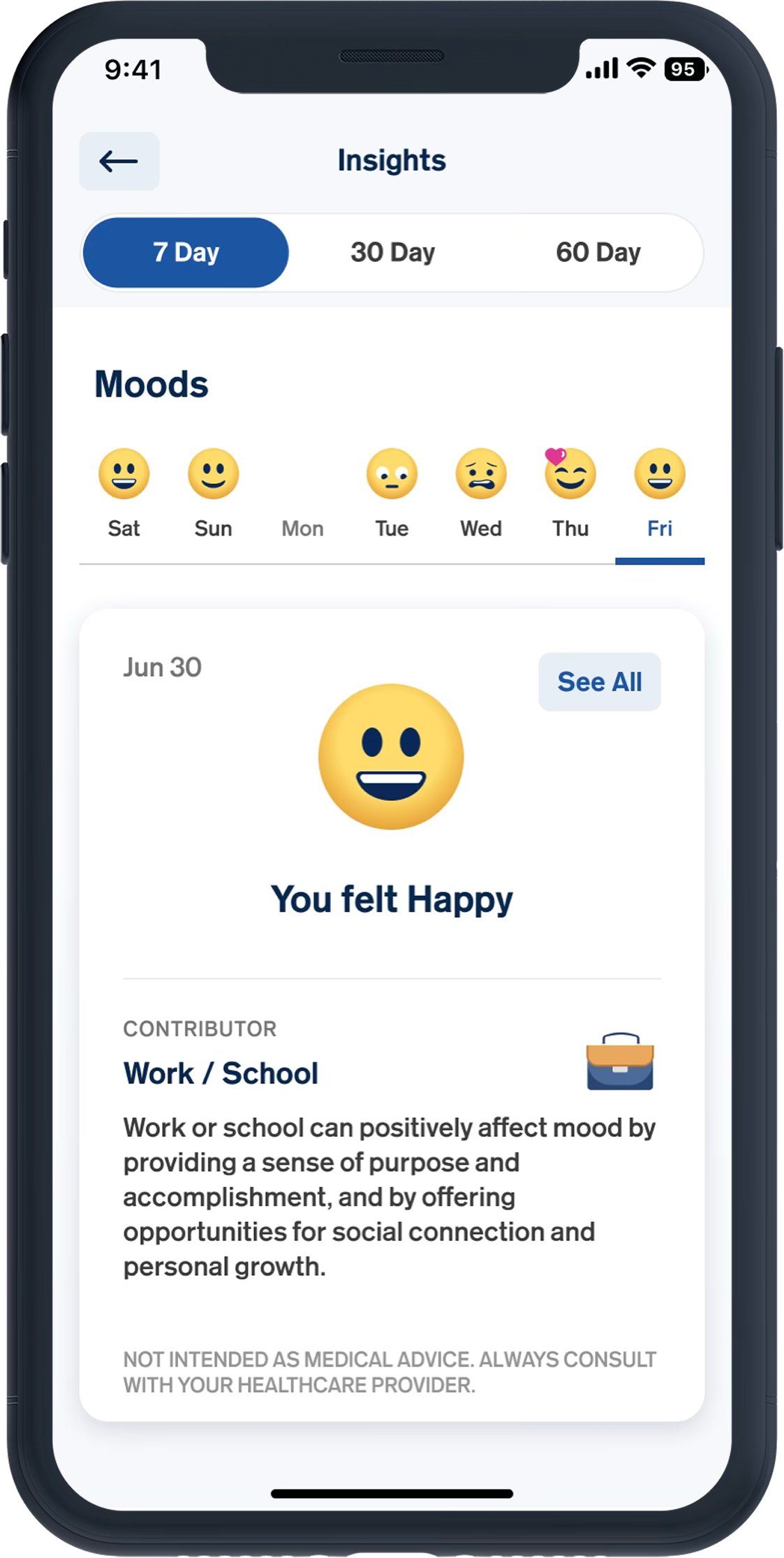
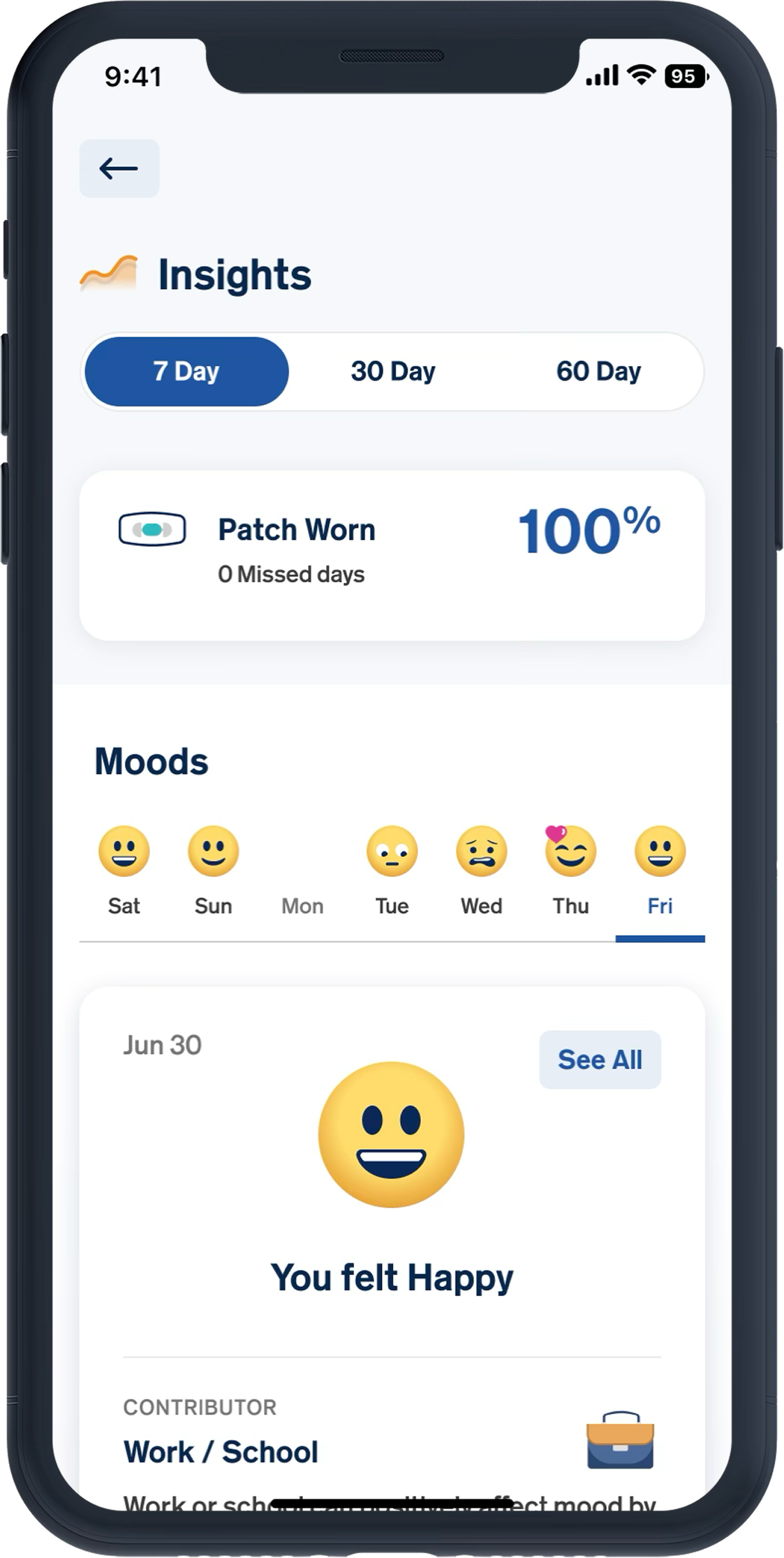
Fear of numeric “proof” of failure
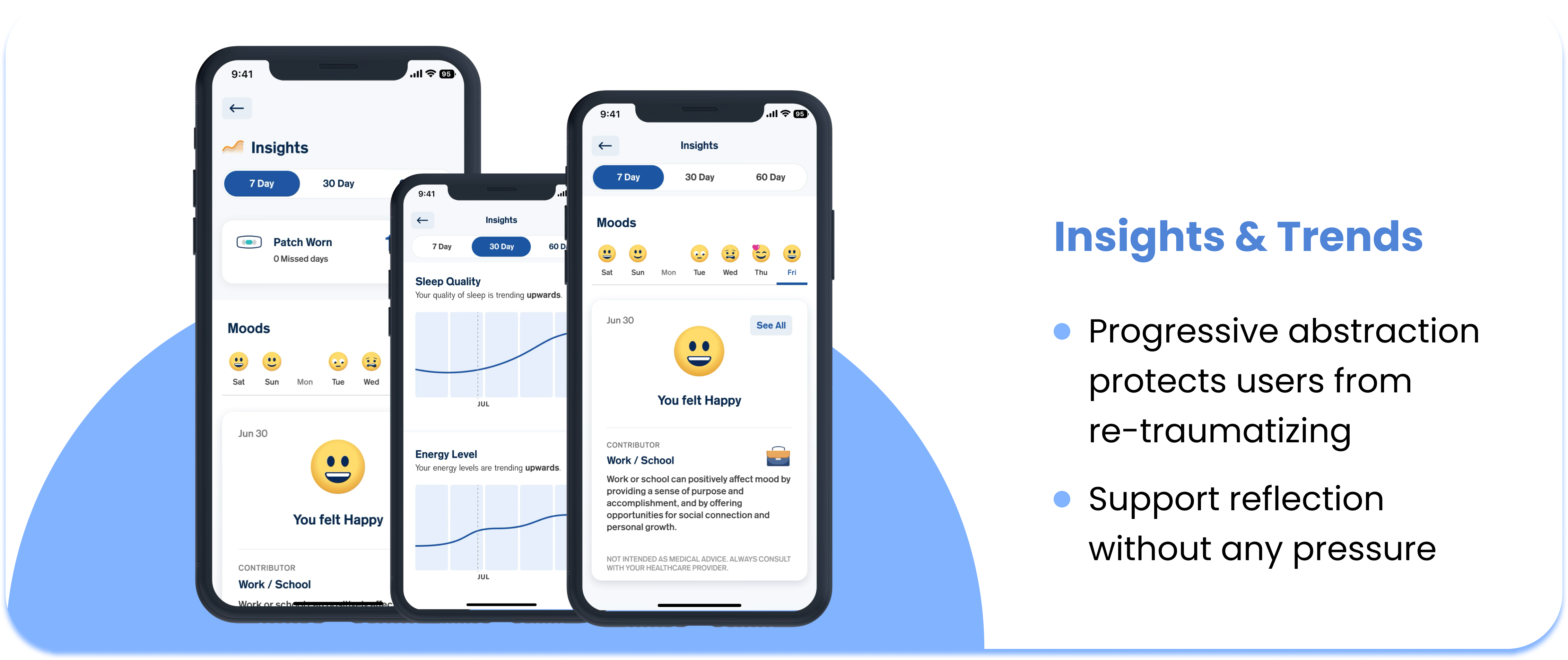
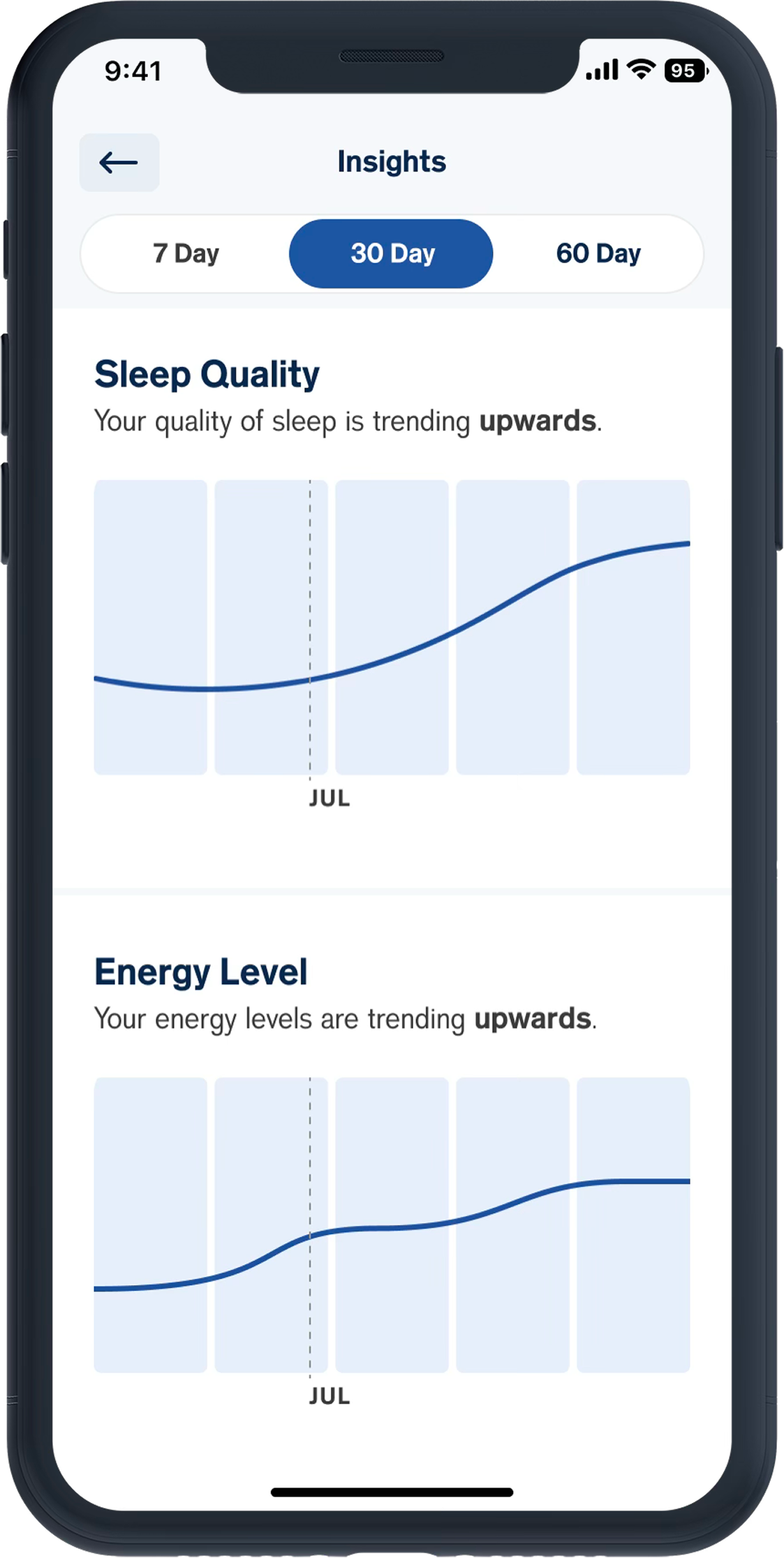
---No percentages, scores, only visual trends
Pattern anxiety
---Progressive abstraction, make data less specific
Clinical-looking charts trigger bad memories
---Soft colors and gentle shapes, avoid clinical design
Comparison to “normal” triggers shame
---No baselines, no “most people feel X” comparisons
Need validation for effort
---Built-in affirmations design
Overwhelm from too much detail
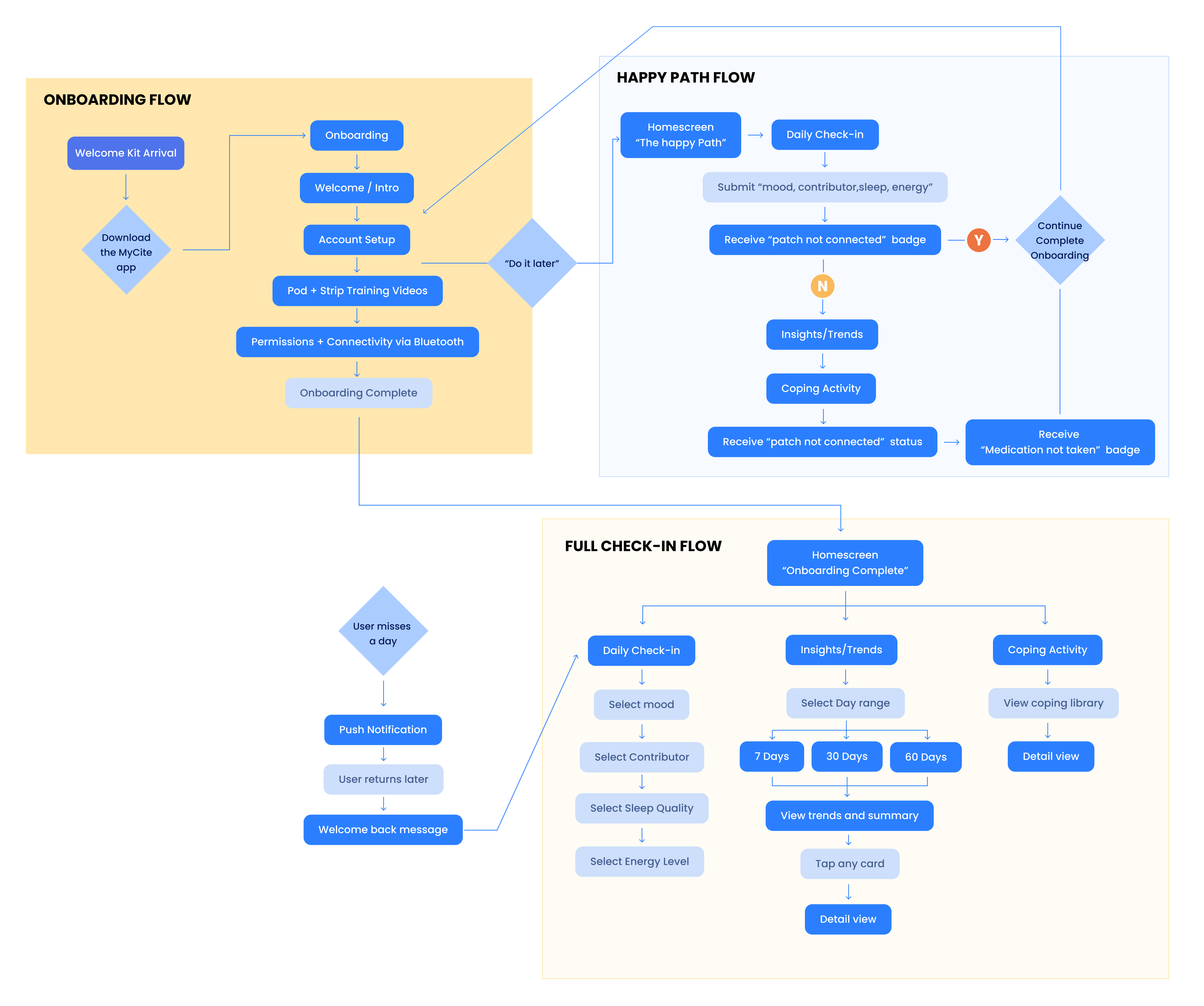
---Divided data into 7/30/60-day views, not showing all at once